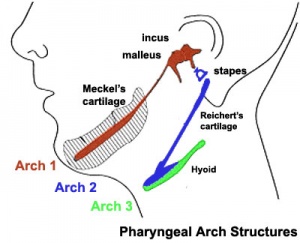
Introduction
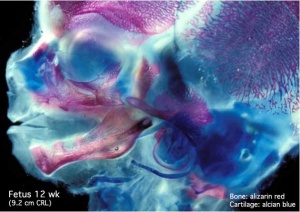
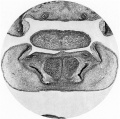
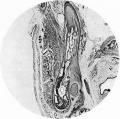
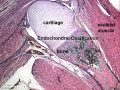
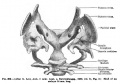
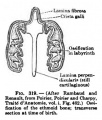
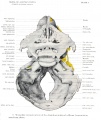
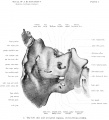
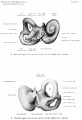
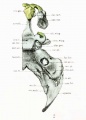
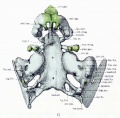
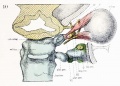
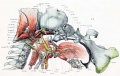
Fetal Head (12 weeks) showing cartilage (blue) and bone (red)
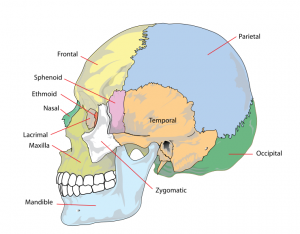
The skull is a unique skeletal structure in several ways: embryonic cellular origin (neural crest and mesoderm), form of ossification (intramembranous and ) and flexibility (fibrous sutures). The cranial vault (which encloses the brain) bones are formed by intramembranous ossification. While the bones that form the base of the skull are formed by endochondral ossification.
Ossification
The bones enclosing the brain have large flexible fibrous joints (sutures) which allow firstly the head to pass through the birth canal and secondly postnatal brain growth. (See also notes on Head Development) In humans, ossification within the skull continues postnatally, through puberty until mid 20's and in old age the sutures separating the vault plates are often completely ossified.
In the entire skeleton, early ossification occurs in the jaw and at the ends of long bones (More? see movie developing mouse). Osteoblasts manufacture bone and are derived from ectomesenchymal in origin. (More? see lineage below). Flexible fibrous sutures allow growth of the brain to be accomodated by calvarial plate growth. Recent studies have show that noggin (a BMP antagonist) is involved in closure of these sutures.
Developmentally and clinically there are several abnormalities associated with skull growth and palate development. These abnormalities can furthermore impact on other systems such as neural, sensory, respiratory and nutritional functions.
Category:Skull | head | neural crest | palate | temporomandibular joint | joint
Some Recent Findings

Historic images of the skull by Vesalius
- Candidate positive targets of LHX6 and LHX8 transcription factors in the developing upper jaw[1] "Craniofacial development is controlled by a large number of genes, which interact with one another to form a complex gene regulatory network (GRN). Key components of GRN are signaling molecules and transcription factors. Therefore, identifying targets of core transcription factors is an important part of the overall efforts toward building a comprehensive and accurate model of GRN. LHX6 and LHX8 are transcription factors expressed in the oral mesenchyme of the first pharyngeal arch (PA1), and they are crucial regulators of palate and tooth development. Previously, we performed genome-wide transcriptional profiling and chromatin immunoprecipitation to identify target genes of LHX6 and LHX8 in PA1, and described a set of genes repressed by LHX. However, there has not been any discussion of the genes positively regulated by LHX6 and LHX8. In this paper, we revisited the above datasets to identify candidate positive targets of LHX in PA1. Focusing on those with known connections to craniofacial development, we performed RNA in situ hybridization to confirm the changes in expression in Lhx6;Lhx8 mutant. We also confirmed the binding of LHX6 to several putative enhancers near the candidate target genes. Together, we have uncovered novel connections between Lhx and other important regulators of craniofacial development, including Eya1, Barx1, Rspo2, Rspo3, and Wnt11."
- Association between the developing sphenoid and adult morphology: A study using sagittal sections of the skull base from human embryos and fetuses[2] "The developing sphenoid is regarded as a median cartilage mass (basisphenoid [BS]) with three cartilaginous processes (orbitosphenoid [OS], ala temporalis [AT], and alar process [AP]). The relationships of this initial configuration with the adult morphology are difficult to determine because of extensive membranous ossification along the cartilaginous elements. The purpose of this study was therefore to evaluate the anatomical connections between each element of the fetal sphenoid and adult morphology. Sagittal sections from 25 embryos and fetuses of gestational age 6-34 weeks and crown-rump length 12-295 mm were therefore examined and compared with horizontal and frontal sections from the other 25 late-term fetuses (217-340 mm). The OS was identified as a set of three mutually attached cartilage bars in early fetuses. At all stages, the OS-post was continuous with the anterolateral part of the BS. The BS included the notochord and Rathke's pouch remnant in embryos and early fetuses. The dorsum sellae was absent from embryos, but it protruded from the BS in early fetuses before a fossa for the hypophysis became evident. Although not higher than the hypophysis at midterm, the dorsum sellae elongated superiorly after gestational age 25 weeks. In early fetuses, the AP was located on the side immediately anterior to the otic capsule. The AT developed on the side immediately posterior to the extraocular rectus muscles. At late term, the greater wing was formed by membranous bones from the AT and AP. The AT and AP formed a complex bridge between the BS and the greater wing. A small cartilage, future medial pterygoid process (PTmed) was located inferior to the AT in early fetuses. At midterm, one endochondral bone and multiple membranous bones formed the PTmed. The lateral pterygoid process (PTlat) was formed by a single membranous bone plate. Therefore, we connected fetal elements and the adult morphology as follows. (1) Derivative of the OS makes not only the lesser wing but also the anterior margin of the body of the sphenoid. (2) Derivatives of the BS are the body of the sphenoid including the sella turcica and the dorsum sellae. (3) Most of the greater wing including the foramen rotundum and the foramen oval originate from the AT and AP and multiple membranous bones. (4) The PTmed originate from endochondral bones and multiple membranous bones, while the PTlat derive from a single membranous bone."
- Review - A comprehensive review of the anterior fontanelle: embryology, anatomy, and clinical considerations.[3] "Fontanelles are a regular feature of infant development in which two segments of bone remain separated, leaving an area of fibrous membrane or a "soft spot" that acts to accommodate growth of the brain without compression by the skull. Of the six fontanelles in the human skull, the anterior fontanelle, located between the frontal and parietal bones, serves as an important anatomical diagnostic tool in the assessment of impairments of the skull and brain and allows access to the brain and ventricles in the infant. The diagnostic value of the anterior fontanelle, through observation of its shape, size, and palpability, makes the area of significant clinical value."
|
| More recent papers
|
|
This table allows an automated computer search of the external PubMed database using the listed "Search term" text link.
- This search now requires a manual link as the original PubMed extension has been disabled.
- The displayed list of references do not reflect any editorial selection of material based on content or relevance.
- References also appear on this list based upon the date of the actual page viewing.
References listed on the rest of the content page and the associated discussion page (listed under the publication year sub-headings) do include some editorial selection based upon both relevance and availability.
More? References | Discussion Page | Journal Searches | 2019 References | 2020 References
Search term: Skull Embryology | Skull Development | Mandible Development
|
| Older papers
|
| These papers originally appeared in the Some Recent Findings table, but as that list grew in length have now been shuffled down to this collapsible table.
See also the Discussion Page for other references listed by year and References on this current page.
- Transcriptional analysis of human cranial compartments with different embryonic origins[4] "Previous investigations suggest that the embryonic origins of the calvarial tissues (neural crest or mesoderm) may account for the molecular mechanisms underlying sutural development. The aim of this study was to evaluate the differences in the gene expression of human cranial tissues and assess the presence of an expression signature reflecting their embryonic origins. Of six paired comparisons, frontal and parietal compartments (distinct tissue types of calvaria, either bone or intrasutural mesenchyme) had the most different gene expression profiles despite being composed of the same tissue type (bone). Transcriptional profiles of two groups of tissues, frontal and metopic compartments vs. parietal and sagittal compartments, suggest differences in proliferation, differentiation and extracellular matrix production. Our data suggest that in the second trimester of human foetal development, a gene expression signature of neural crest origin still exists in frontal and metopic compartments while gene expression of parietal and sagittal compartments is more similar to mesoderm."
- The BMP Ligand Gdf6 Prevents Differentiation of Coronal Suture Mesenchyme in Early Cranial Development[5] "Growth Differentiation Factor-6 (Gdf6) is a member of the Bone Morphogenetic Protein (BMP) family of secreted signaling molecules. Previous studies have shown that Gdf6 plays a role in formation of a diverse subset of skeletal joints. In mice, loss of Gdf6 results in fusion of the coronal suture, the intramembranous joint that separates the frontal and parietal bones. .... Therefore, although BMPs are known to promote bone formation, Gdf6 plays an inhibitory role to prevent the osteogenic differentiation of the coronal suture mesenchyme."
- Epigenetic control of skull morphogenesis by histone deacetylase 8[6] "Histone deacetylases (Hdacs) are transcriptional repressors with crucial roles in mammalian development. Here we provide evidence that Hdac8 specifically controls patterning of the skull by repressing a subset of transcription factors in cranial neural crest cells. Global deletion of Hdac8 in mice leads to perinatal lethality due to skull instability, and this is phenocopied by conditional deletion of Hdac8 in cranial neural crest cells. Hdac8 specifically represses the aberrant expression of homeobox transcription factors such as Otx2 and Lhx1. These findings reveal how the identity and patterning of vertebrate-specific portions of the skull are epigenetically controlled by a histone deacetylase."
- Expression of five frizzleds during zebrafish craniofacial development.[7] "Wnt/Planar Cell Polarity (PCP) signaling is critical for proper animal development. ...Frizzled (Fzd) homologues are Wnt receptors ...Closer examination revealed that fzd7b is expressed in the neural crest and the mesodermal core of the pharyngeal arches and in the chondrocytes of newly stacked craniofacial cartilage elements. However, fzd7a is only expressed in the neural crest of the pharyngeal arches and fzd8a is expressed in the pharyngeal endoderm."
- Skull Abnormalities - Craniosynostosis[8] "Craniosynostosis, the fusion of one or more of the sutures of the skull vault before the brain completes its growth, is a common (1 in 2,500 births) craniofacial abnormality, approximately 20% of which occurrences are caused by gain-of-function mutations in FGF receptors (FGFRs). ...These experiments show that attenuation of FGFR signaling by pharmacological intervention could be applied for the treatment of craniosynostosis or other severe bone disorders caused by mutations in FGFRs that currently have no treatment."
|
Fetal Skull
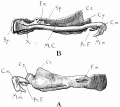
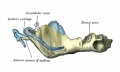
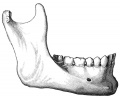
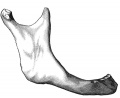
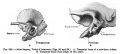
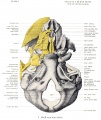
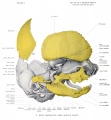
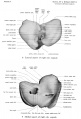
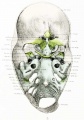
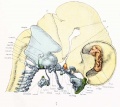
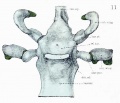
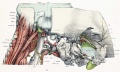
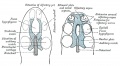
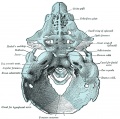
The Images below show the combined endochondral and intramembranous ossification that is occurring in early fetal development (week 12).
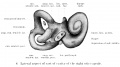
In the first 2 images the bone cartilage is shown in blue and the new bone in red.
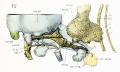
Note the difference in appearance between the upper and lower jaw (maxilla and mandible), the currently cartilage base of the skull (chondrocranium) and the cranial vault (neurocranium).
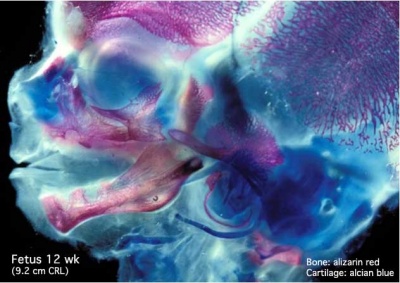
Fetal head lateral view
|
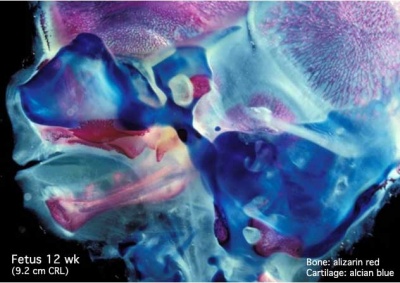
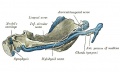
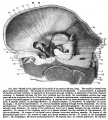
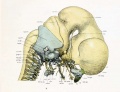
Fetal head medial view
|
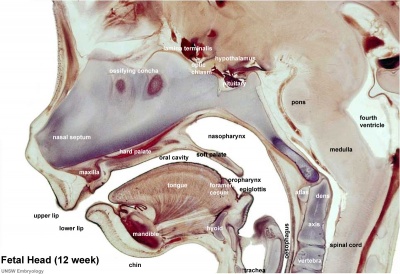
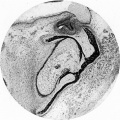
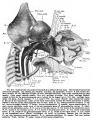
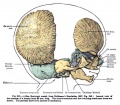
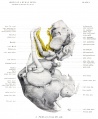
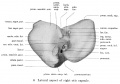
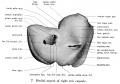
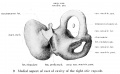
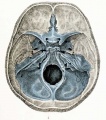
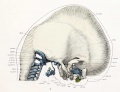
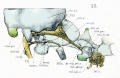
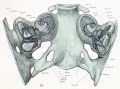
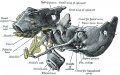
Fetal head section
|
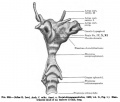
This mid-line section through the fetal head shows features of the developing skull and the brain, face and mouth.
- Neural
- developing brain and brainstem.
- lamina terminalis (site of anterior neuropore closure).
- fourth ventricle.
- developing pituitary sitting in the sella turcica.
- Musculoskeletal
- cartilage - septum of the nose.
- bone - ossifying nasal concha.
- bone - palate roof of mouth.
- cartilage - soft palate back of mouth.
- cartilage - base of skull and vertebra.
- muscle - tongue, attached note foramen cecum.
- bone - mandible.
- cartilage - developing hyoid and thyroid bones.
|
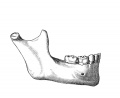
Mandible Development
Meckel's cartilage, located within the first pharyngeal arch mandibular prominence, forms a cartilage "template" besides which the mandible bone develops by the process of intramembranous ossification. It is important to note that this cartilage template does not ossify (endochondral ossification) but provides a transient structure where the mandible will form, and later degenerates.
See also the 1957 historic paper on temporomandibular joint development.[9]
Embryonic and Fetal Mandible
Birth to Adult Mandible
|
|

Animated GIF
|
- Mandible Development: Week 8 outer view | Week 8 inner view | Week 12 outer view | Week 12 inner view | Week 12 Head outer view | Week 12 Head inner view | Birth | Childhood | Adult | Old Age | Small Animation | Large Animation | Muscle Attachments | Mandible Ossification | 1909 Mandible | embryo 18 mm | embryo 24 mm | embryo 28 mm | fetus 43 mm | fetus 65 mm | fetus 55 mm | fetus 95 mm | human 18-24-95 mm | Skull Development | Head Development
- Links: Temporomandibular Joint Development
Neurocranium
Frontal bone
- neural crest origin
- requires Msx1 and Dlx5[10]
Parietal bone
Skull Views
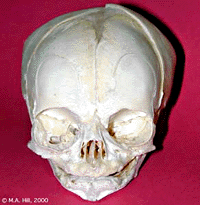
|

|

|
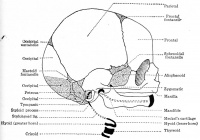
|
| anterior view
|
superior view
|
lateral view
|
lateral view
|
| showing anterior fontenelle, sutures, mandible
|
showing anterior fontenelle, sutures
|
showing suture, mandible
|
newborn skull
|
Skull Fontanels and Sutures
The bones enclosing the brain have large flexible fibrous joints (sutures) which allow firstly the head to compress and pass through the birth canal and secondly to postnatally expand for brain growth. (More? Molecular Skull Sutures) These sutures gradually fuse at different times postnatally, firstly the metopic suture in infancy and the others much later. Abnormal fusion (synostosis) of any of the sutures will lead to a number of different skull defects, leading to disruption of brain development. (More? Abnormal Synostosis) In old age all these sutures are generally completely fused and ossified.
Skull Fontanels
The newborn skull has 6 fontanels (fontanelles) the most obvious are the anterior and posterior fontanels that close at different times postnatally.
- posterior fontanel closes at about 3 months
- anterior fontanel closes at about 18 months
|
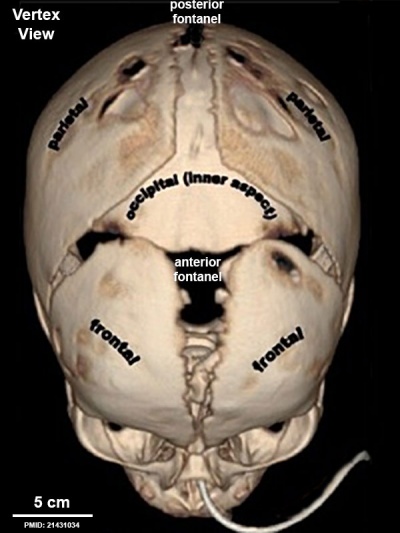
Newborn Skull Fontanels (CT, vertex view)
|
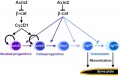
At the molecular level, accelerated suture intramembranous ossification can be mediated through a dual role of β-catenin in both the expansion of osteoprogenitors and the maturation of osteoblasts.[11] These researchers also show that disruption of Axin2/β-catenin signaling alters the regulation of the downstream transcription target, cyclin D1, in the canonical Wnt pathway.[12]
Computed Tomography Views
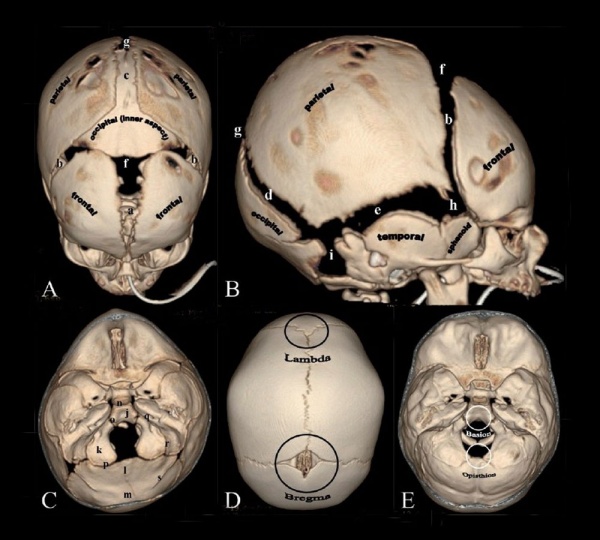
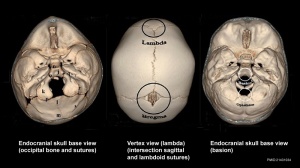
Skull CT Vertex, later and basal views.[13]
|
Sutures and Fontanels
- a - Metopic suture
- b - coronal sutures
- c - sagittal suture
- d - lambdoid suture
- e - squamosal suture
- f - anterior fontanel
- g - posterior fontanel
- h - sphenoidal fontanel
- i - mastoid fontanel
|
coronal suture
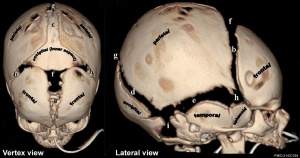
lambdoid suture
metopic suture begins at nose and runs superiorly to meet sagittal suture and fuses during infancy (fusion beginning at 3 months and completes by 6 to 8 months of age) before all other cranial sutures.
sagittal suture
Cranial Base Synchondroses
In the base of the skull there can also be found a number of synchondrosis, "cartilage sutures", that are the last to close and have a role in the ongoing growth of the postnatal skull. Synchondrosis is a type of cartilaginous joint in which the cartilage is usually converted into bone before adult life. It has been compared in appearance to a long bone growth plate, but is bipolar rather than unipolar in structure.
These sutures also lost at different times in postnatal development:
- Inter-sphenoidal – around birth
- Spheno-ethmoidal – 6-7 yrs
- Spheno-occipital – 12-15 yrs
Fetal Head Growth
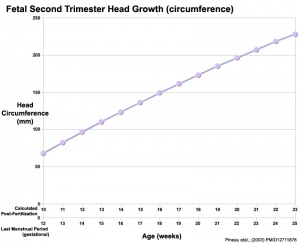
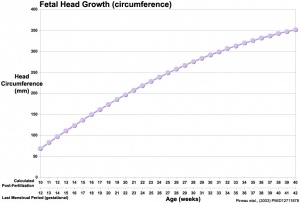
Abnormalities
There are several skull deformities caused by premature fusion (synostosis) of different developing skull sutures. Suture abnormalities are classified as either "simple" (only one suture involved) or "compound" (two or more sutures involved). Failure of neural (brain) development may also result in acrocephaly of the skull.
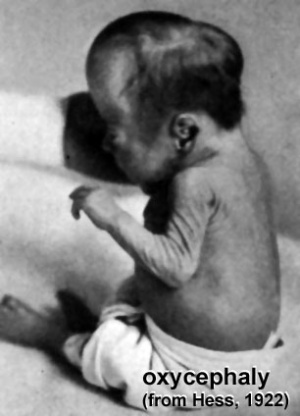 Oxycephalus (historic image from Hess, 1922)
Oxycephalus (historic image from Hess, 1922)
|
* craniosynostosis premature cranial suture fusion, results in an abnormal skull shape, blindness and mental retardation.
- oxycephaly (tower skull) results from premature coronal suture synostosis.
- plagiocephaly results from asymmetric coronal suture synostosis, incidence is approximately 1 in 300 live births.
- lambdoid synostosis results from premature lambdoid suture synostosis, a rare abnormality (incidence is approximately 3 in 100,000 live births) which displaces ear posteriorly towards the fused suture.
- caphocephaly results from premature sagittal suture synostosis.
- trigoncephaly (wedge skull) results from metopic suture synostosis.
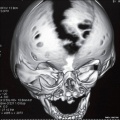
The CT images shown below are from a recent review of skull abnormalities.[13]
|
Craniosynostosis
Attenuation of signaling pathways stimulated by pathologically activated FGF-receptor 2 mutants prevents craniosynostosis.[8] "Craniosynostosis, the fusion of one or more of the sutures of the skull vault before the brain completes its growth, is a common (1 in 2,500 births) craniofacial abnormality, approximately 20% of which occurrences are caused by gain-of-function mutations in FGF receptors (FGFRs). ...These experiments show that attenuation of FGFR signaling by pharmacological intervention could be applied for the treatment of craniosynostosis or other severe bone disorders caused by mutations in FGFRs that currently have no treatment."
See also Crouzon syndrome.
Dolichocephaly and scaphocephaly
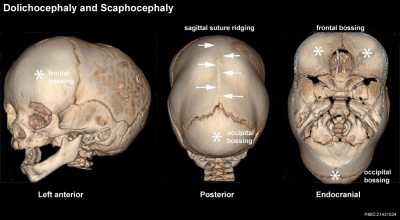
|
| Dolichocephaly and scaphocephaly
(premature fusion of the sagittal suture)
|
Brachycephaly and anterior plagiocephaly
(Greek, brakhu = short) (Greek plagios = oblique)
- brachycephaly - premature bicoronal fusion
- anterior plagiocephaly - unicoronal fusion
Leads to a restriction of anterior-posterior calvarial growth and relatively unaffected biparietal growth.
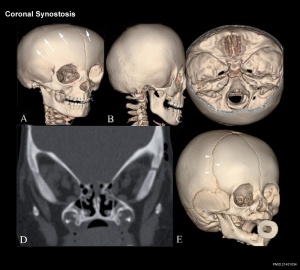
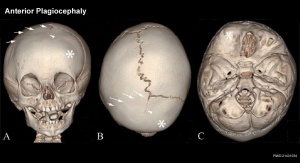
Skull Turricephaly
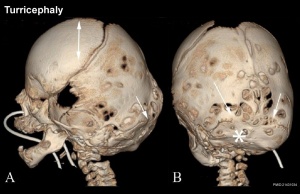
Skull Trigonocephaly
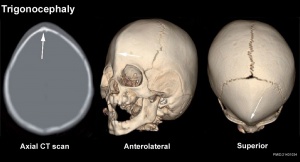
(Greek, trigonos = three angles) This abnormality results from the premature fusion of the metopic suture occurring before 6 months (3-9 months) of age.
Skull Oxycephaly
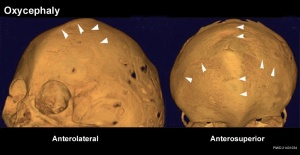
Images show oxycephaly from severe sagittal and coronal synostoses (arrowheads).
Craniofrontonasal Syndrome
Craniofrontonasal syndrome (CFNS) is a human X-linked developmental disorder caused by a mutation in ephrin-B1 affecting mainly females. Characterised by abnormal development of cranial and nasal bones, craniosynostosis (premature coronal suture fusion), and other extracranial anomalies (limb polydactyly and syndactyly).

|
(a) Facial view showing marked hypertelorism, divergent squint, and central nasal groove (subject age, 1 year).
(b) Three-dimensional computed tomographic skull reconstruction (subject age, 8 months) showing right unicoronal synostosis, lateral displacement of orbits, and central defect between frontal bones. Note bony ridge at site of obliterated right coronal suture (arrowhead); the left coronal suture is patent (arrow). f, frontal bone; p, parietal bone.
(c) Longitudinal splitting of the nails is frequent.
|
| Craniofrontonasal syndrome[14]
|
Links: OMIM - Craniofrontonasal Syndrome
|
Crouzon syndrome
Crouzon syndrome (craniofacial dysostosis) rare genetic disorder also characterized by premature closure of cranial sutures. Cranial and facial malformations vary, ranging from mild to potentially severe, including among members of the same family (autosomal dominant). The syndrome is caused by mutations in one of the FGFR genes, most commonly FGFR2.
- Links: OMIM - FGFR2
Skull Histology
A histological image of a skull bone formation by Intramembranous ossification.
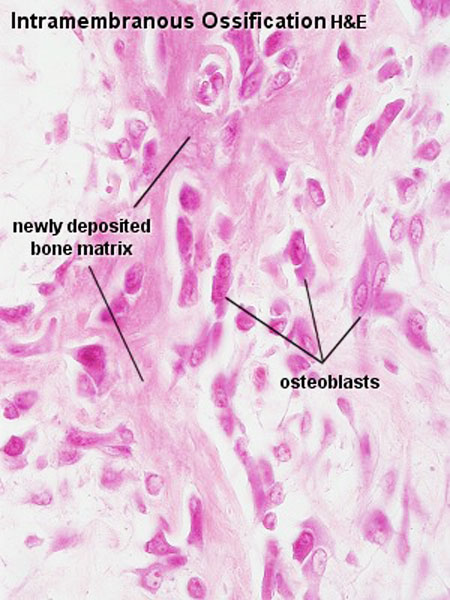
Adult Skull
References
- ↑ Cesario J, Ha S, Kim J, Kataria N & Jeong J. (2021). Candidate positive targets of LHX6 and LHX8 transcription factors in the developing upper jaw. Gene Expr Patterns , 43, 119227. PMID: 34861428 DOI.
- ↑ Yamamoto M, Jin ZW, Hayashi S, Rodríguez-Vázquez JF, Murakami G & Abe S. (2021). Association between the developing sphenoid and adult morphology: A study using sagittal sections of the skull base from human embryos and fetuses. J Anat , 239, 1300-1317. PMID: 34268732 DOI.
- ↑ D'Antoni AV, Donaldson OI, Schmidt C, Macchi V, De Caro R, Oskouian RJ, Loukas M & Shane Tubbs R. (2017). A comprehensive review of the anterior fontanelle: embryology, anatomy, and clinical considerations. Childs Nerv Syst , 33, 909-914. PMID: 28396968 DOI.
- ↑ Homayounfar N, Park SS, Afsharinejad Z, Bammler TK, MacDonald JW, Farin FM, Mecham BH & Cunningham ML. (2015). Transcriptional analysis of human cranial compartments with different embryonic origins. Arch. Oral Biol. , 60, 1450-60. PMID: 26188427 DOI.
- ↑ Clendenning DE & Mortlock DP. (2012). The BMP ligand Gdf6 prevents differentiation of coronal suture mesenchyme in early cranial development. PLoS ONE , 7, e36789. PMID: 22693558 DOI.
- ↑ Haberland M, Mokalled MH, Montgomery RL & Olson EN. (2009). Epigenetic control of skull morphogenesis by histone deacetylase 8. Genes Dev. , 23, 1625-30. PMID: 19605684 DOI.
- ↑ Sisson BE & Topczewski J. (2009). Expression of five frizzleds during zebrafish craniofacial development. Gene Expr. Patterns , 9, 520-7. PMID: 19595791 DOI.
- ↑ 8.0 8.1 Eswarakumar VP, Ozcan F, Lew ED, Bae JH, Tomé F, Booth CJ, Adams DJ, Lax I & Schlessinger J. (2006). Attenuation of signaling pathways stimulated by pathologically activated FGF-receptor 2 mutants prevents craniosynostosis. Proc. Natl. Acad. Sci. U.S.A. , 103, 18603-8. PMID: 17132737 DOI.
- ↑ Moffatt BC. The prenatal development of the human temporomandibular joint. (1957) Carnegie Instn. Wash. Publ. 611, Contrib. Embryol., 36: .
- ↑ Chung IH, Han J, Iwata J & Chai Y. (2010). Msx1 and Dlx5 function synergistically to regulate frontal bone development. Genesis , 48, 645-55. PMID: 20824629 DOI.
- ↑ Liu B, Yu HM & Hsu W. (2007). Craniosynostosis caused by Axin2 deficiency is mediated through distinct functions of beta-catenin in proliferation and differentiation. Dev. Biol. , 301, 298-308. PMID: 17113065 DOI.
- ↑ Mirando AJ, Maruyama T, Fu J, Yu HM & Hsu W. (2010). β-catenin/cyclin D1 mediated development of suture mesenchyme in calvarial morphogenesis. BMC Dev. Biol. , 10, 116. PMID: 21108844 DOI.
- ↑ 13.0 13.1 Khanna PC, Thapa MM, Iyer RS & Prasad SS. (2011). Pictorial essay: The many faces of craniosynostosis. Indian J Radiol Imaging , 21, 49-56. PMID: 21431034 DOI.
- ↑ Twigg SR, Kan R, Babbs C, Bochukova EG, Robertson SP, Wall SA, Morriss-Kay GM & Wilkie AO. (2004). Mutations of ephrin-B1 (EFNB1), a marker of tissue boundary formation, cause craniofrontonasal syndrome. Proc. Natl. Acad. Sci. U.S.A. , 101, 8652-7. PMID: 15166289 DOI.
Reviews
Liao J, Huang Y, Wang Q, Chen S, Zhang C, Wang D, Lv Z, Zhang X, Wu M & Chen G. (2022). Gene regulatory network from cranial neural crest cells to osteoblast differentiation and calvarial bone development. Cell Mol Life Sci , 79, 158. PMID: 35220463 DOI.
Shah M, Ross JS, VanDyke C, Rudick RA, Goodkin DE, Obuchowski N & Modic MT. (1992). Volume T1-weighted gradient echo MRI in multiple sclerosis patients. J Comput Assist Tomogr , 16, 731-6. PMID: 1522265
Stelnicki EJ, Mooney MP, Losken HW, Zoldos J, Burrows AM, Kapucu R & Siegel MI. (1997). Ultrasonic prenatal diagnosis of coronal suture synostosis. J Craniofac Surg , 8, 252-8; discussion 259-61. PMID: 9482048
Ocampo RV & Persing JA. (1994). Sagittal synostosis. Clin Plast Surg , 21, 563-74. PMID: 7813156
Vander Kolk CA & Carson BS. (1994). Lambdoid synostosis. Clin Plast Surg , 21, 575-84. PMID: 7813157
Cohen MM. (1993). Sutural biology and the correlates of craniosynostosis. Am. J. Med. Genet. , 47, 581-616. PMID: 8266985 DOI.
Articles
Weinzweig J, Kirschner RE, Farley A, Reiss P, Hunter J, Whitaker LA & Bartlett SP. (2003). Metopic synostosis: Defining the temporal sequence of normal suture fusion and differentiating it from synostosis on the basis of computed tomography images. Plast. Reconstr. Surg. , 112, 1211-8. PMID: 14504503 DOI.
Search PubMed
Search July 2010 "Skull Development" All (15473) Review (1231) Free Full Text (1634)
Search Pubmed: Skull Development
Additional Images
Skull - osteoblast lineage model
Skull vault defect and midface hypoplasia
Historic
Historic Embryology
| Johns Hopkins Fetal Skull Collection (1918–1951)
|
| Johns Hopkins Fetal Skull Collection (1918–1951) - Simplified | Simplified Collapse | Full | Skull Development
|
| Specimen
|
Schultz Number
|
Schultz Number (Old)
|
Sex
|
Race
|
Ted Combs Age 1
|
Ted Combs Age 2
|
Ted Combs Notes
|
| JH 001
|
6
|
Blank
|
Male
|
B
|
5-6
|
IU
|
Left Occipital Condyle Missing 7/01 JR
|
| JH 002
|
15
|
253
|
Male
|
B
|
7
|
IU
|
|
| JH 003
|
18
|
Blank
|
Male
|
B
|
11
|
PN
|
LEFT GREATER WING MAY HAVE BEEN BROKEN
|
| JH 004
|
34
|
394
|
Male
|
B
|
12
|
PN
|
ENTIRE BASICRANIUM FUSED
|
| JH 005
|
35
|
361
|
Male
|
B
|
10
|
IU
|
|
| JH 006
|
36
|
258
|
Male
|
B
|
7
|
IU
|
ADOLF H SCHULTZ DRAWING INCLUDED
|
| JH 007
|
38
|
269
|
Male
|
B
|
10-11
|
IU
|
IMPROPER OSSIFICATION OF DORSUM STELLA
|
| JH 008
|
51
|
Blank
|
Male
|
B
|
5
|
IU
|
NOT ALL BONES BELONG HERE
|
| JH 009
|
56
|
271
|
Male
|
B
|
10
|
IU
|
|
| JH 010
|
58
|
340
|
Male
|
B
|
9-10
|
IU
|
|
| JH 011
|
62
|
Blank
|
Male
|
B
|
0
|
Newborn
|
|
| JH 012
|
67
|
322
|
Male
|
B
|
0
|
Newborn
|
MOLAR BUDS INCLUDED
|
| JH 013
|
69
|
299
|
Male?
|
B
|
9
|
IU
|
CHECK SEX
|
| JH 014
|
71
|
323
|
Male
|
B
|
0
|
Newborn
|
|
| JH 015
|
78
|
298
|
Male
|
B
|
8
|
IU
|
IMPROPER OSSIFICATION OF THE STELLA TURCICA
|
| JH 016
|
83
|
Blank
|
Male
|
B
|
7
|
IU
|
|
| JH 017
|
91
|
334
|
Male
|
B
|
10
|
IU
|
|
| JH 018
|
96
|
310
|
Male
|
B
|
10
|
IU
|
SQUAMOUS PORTION OF OCCIPITAL IN 2 PIECES
|
| JH 019
|
109
|
315
|
Male
|
B
|
10
|
IU
|
EXTRA BROKEN MALLEUS INCLUDED
|
| JH 020
|
110
|
257
|
Male
|
B
|
6
|
IU
|
TEMPORALS POORLY OSSIFIED
|
| JH 021
|
111
|
342
|
Male
|
B
|
3
|
PN
|
|
| JH 022
|
126
|
367
|
Male
|
B
|
10
|
IU
|
|
| JH 023
|
135
|
250
|
Male
|
B
|
8
|
IU
|
VERY YOUNG
|
| JH 024
|
137
|
285
|
Male
|
B
|
8
|
IU
|
|
| JH 025
|
139
|
400
|
Male
|
B
|
0
|
Newborn
|
|
| JH 026
|
144
|
Blank
|
Male
|
B
|
10
|
IU
|
"Two right lateral occipital bones and no left
JR 7/12/2001"
|
| JH 027
|
147
|
391
|
Male
|
B
|
2
|
PN
|
LEFT FRONTAL IS THE ONLY BONE PRESENT.
|
| JH 028
|
155
|
355
|
Male
|
B
|
0
|
Newborn
|
|
| JH 029
|
159
|
273
|
Male
|
B
|
9
|
IU
|
|
| JH 030
|
161
|
367
|
Male
|
B
|
0
|
Newborn
|
|
| JH 031
|
164
|
359
|
Male
|
B
|
2
|
PN
|
MANDIBLE ONCE FUSED, NOW BROKEN"
|
| JH 032
|
178
|
483
|
Male
|
B
|
15
|
PN
|
MaleOST OF BASICRANIUM FUSED
|
| JH 033
|
184
|
365
|
Male
|
B
|
2
|
PN
|
|
| JH 034
|
189
|
377
|
Male
|
B
|
3
|
PN
|
|
| JH 035
|
2
|
306
|
Female
|
B
|
0
|
Newborn
|
MANDIBLE WAS FUSED: NOW BROKEN
|
| JH 036
|
8
|
Blank
|
Female
|
B
|
9
|
IU
|
|
| JH 037
|
14
|
236
|
Female
|
B
|
5
|
IU
|
|
| JH 038
|
17
|
Blank
|
Female
|
B
|
14
|
PN
|
ADOLF H SCHULTZ DRAWING INCLUDED
|
| JH 039
|
44
|
298
|
Female
|
B
|
8
|
IU
|
EXTRA MALLEUS
|
| JH 040
|
45
|
Blank
|
Female
|
B
|
0
|
Newborn
|
POOR OSSIFICATION OF THE CALVARIA
|
| JH 041
|
53
|
440
|
Female
|
B
|
12
|
PN
|
WHOLE SKULL BADLY OSSIFIED
|
| JH 042
|
57
|
366
|
Female
|
B
|
2
|
PN
|
|
| JH 043
|
59
|
Blank
|
Female
|
B
|
8
|
IU
|
|
| JH 044
|
61
|
340
|
Female
|
B
|
9
|
IU
|
INCOMPLETE
|
| JH 045
|
63
|
340BUG!!!
|
Female
|
B
|
12
|
PN
|
TEETH BELONG TO JH 05. BAD BONE.
|
| JH 046
|
70
|
345
|
Female
|
B
|
3
|
PN
|
|
| JH 047
|
75
|
364
|
Female
|
B
|
0
|
Newborn
|
|
| JH 048
|
84
|
Blank
|
Female
|
B
|
8
|
IU
|
|
| JH 049
|
86
|
341
|
Female
|
B
|
2
|
PN
|
|
| JH 050
|
88
|
294
|
Female
|
B
|
8
|
IU
|
|
| JH 051
|
101
|
290
|
Female
|
B
|
8
|
IU
|
|
| JH 052
|
107
|
Blank
|
Female
|
B
|
8
|
IU
|
|
| JH 053
|
118
|
311
|
Female
|
B
|
9
|
IU
|
NASAL BONES FUSED
|
| JH 054
|
120
|
252
|
Female
|
B
|
8
|
IU
|
|
| JH 055
|
121
|
276
|
Female
|
B
|
6
|
IU
|
|
| JH 056
|
122
|
313
|
Female
|
B
|
?
|
?
|
TWO FRONTALS FROM TWO SPECIMENS (SIDES IN DISPUTE) EAR OSSICLES WITH SMALL....(?)
|
| JH 057
|
127
|
307
|
Female
|
B
|
10
|
IU
|
|
| JH 058
|
132
|
354
|
Female
|
B
|
4
|
PN
|
|
| JH 059
|
149
|
290
|
Female
|
B
|
8
|
IU
|
|
| JH 060
|
150
|
2825
|
Female
|
B
|
See Note
|
See Note
|
Age estimated as 8 months to Newborn
|
| JH 061
|
169
|
340
|
Female
|
B
|
0
|
Newborn
|
|
| JH 062
|
172
|
283
|
Female
|
B
|
7
|
IU
|
|
| JH 063
|
185
|
345
|
Female
|
B
|
10
|
IU
|
|
| JH 064
|
190
|
331
|
Female
|
B
|
2
|
PN
|
|
| JH 065
|
191
|
256
|
Female
|
B
|
5-6
|
IU
|
|
| JH 066
|
10
|
240
|
Male
|
W
|
5
|
IU
|
|
| JH 067
|
20
|
Blank
|
Male
|
W
|
0
|
Newborn
|
Reported missing by JR 7/001
|
| JH 068
|
40
|
Blank
|
Male
|
W
|
2
|
PN
|
|
| JH 069
|
48
|
340
|
Male
|
W
|
7
|
IU
|
|
| JH 070
|
49
|
274
|
Male
|
W
|
6-7
|
IU
|
|
| JH 071
|
74
|
332
|
Male
|
W
|
10
|
IU
|
|
| JH 072
|
77
|
336
|
Male
|
W
|
10
|
IU
|
|
| JH 073
|
89
|
344
|
Male
|
W
|
9
|
IU
|
|
| JH 074
|
92
|
279
|
Male
|
W
|
6
|
IU
|
|
| JH 075
|
105
|
Blank
|
Male
|
W
|
6
|
IU
|
|
| JH 076
|
108
|
280
|
Male
|
W
|
9
|
IU
|
|
| JH 077
|
129
|
340
|
Male
|
W
|
1
|
PN
|
|
| JH 078
|
131
|
364
|
Male
|
W
|
9
|
IU
|
|
| JH 079
|
136
|
363
|
Male
|
W
|
9
|
IU
|
|
| JH 080
|
138
|
355
|
Male
|
W
|
3
|
PN
|
KERKRING'S CENTER OBSERVED
|
| JH 081
|
141
|
347
|
Male
|
W
|
2
|
PN
|
MANDIBLE ONCE FUSED NOW BROKEN
|
| JH 082
|
143
|
326
|
Male
|
W
|
0
|
Newborn
|
EXTRA MALLEUS INCLUDED
|
| JH 083
|
146
|
320
|
Male
|
W
|
9
|
IU
|
THREE PARIETAL FRAGMENTS
|
| JH 084
|
151
|
353
|
Male
|
W
|
3
|
PN
|
|
| JH 085
|
156
|
364
|
Male
|
W
|
2
|
PN
|
|
| JH 086
|
157
|
288
|
Male
|
W
|
8
|
IU
|
|
| JH 087
|
162
|
374
|
Male
|
W
|
9
|
IU
|
|
| JH 088
|
166
|
382
|
Male
|
W
|
4
|
PN
|
MANY TOOTH FRAGMENTS
|
| JH 089
|
171
|
380
|
Male
|
W
|
10
|
IU
|
NASAL BONES FUSED
|
| JH 090
|
179
|
Blank
|
Male
|
W
|
3
|
PN
|
|
| JH 091
|
186
|
373
|
Male
|
W
|
9
|
IU
|
|
| JH 092
|
188
|
Blank
|
Male
|
W
|
8
|
IU
|
|
| JH 093
|
192
|
328
|
Male
|
W
|
7
|
IU
|
KERKRING'S CENTER OBSERVED
|
| JH 094
|
13
|
Blank
|
Female
|
W
|
0
|
Newborn
|
TEETH FRAGMENTS
|
| JH 095
|
23
|
352
|
Female
|
W
|
4
|
PN
|
TYMPANIC MEMBRANE INTACT
|
| JH 096
|
43
|
268
|
Female
|
W
|
5
|
IU
|
ADOLF H SCHULTZ DRAWING INCLUDED
|
| JH 097
|
47
|
313
|
Female
|
W
|
8
|
IU
|
ONE BONE FRAGMENT - SQUAMOUS TYPE
|
| JH 098
|
64
|
364
|
Female
|
W
|
3
|
PN
|
|
| JH 099
|
95
|
350
|
Female
|
W
|
4
|
PN
|
HYDROCEPHALIC
|
| JH 100
|
100
|
365
|
Female
|
W
|
0
|
Newborn
|
|
| JH 101
|
114
|
396
|
Female
|
W
|
5
|
PN
|
MANDIBLE ONCE FUSED NOW BROKEN
|
| JH 102
|
116
|
400
|
Female
|
W
|
2
|
PN
|
TEETH NOT COUNTED
|
| JH 103
|
117
|
290
|
Female
|
W
|
7
|
IU
|
TWO TOOTH BUDS
|
| JH 104
|
128
|
368
|
Female
|
W
|
5
|
PN
|
TOOTH FRAGMENTS
|
| JH 105
|
134
|
Blank
|
Female
|
W
|
9
|
IU
|
EAR OSSICLES PRESENT - NO COUNT
|
| JH 106
|
148
|
290
|
Female
|
W
|
8
|
IU
|
EAR OSSICLES PRESENT - NO COUNT
|
| JH 107
|
160
|
60
|
Female
|
W
|
2
|
PN
|
EAR OSSICLES PRESENT - NO COUNT
|
| JH 108
|
167
|
372
|
Female
|
W
|
1
|
PN
|
EAR OSSICLES PRESENT - NO COUNT
|
| JH 109
|
168
|
316
|
Female
|
W
|
8
|
IU
|
EAR OSSICLES PRESENT - NO COUNT
|
| JH 110
|
170
|
331
|
Female
|
W
|
0
|
Newborn
|
EAR OSSICLES PRESENT - NO COUNT
|
| JH 111
|
175
|
342
|
Female
|
W
|
10
|
IU
|
EAR OSSICLES PRESENT - NO COUNT
|
| JH 112
|
194
|
317
|
Female
|
W
|
8
|
IU
|
|
| Johns Hopkins Fetal Skull Collection (1918–1951) - The collection was begun by Adolph Hans Schultz (1891–1976) - fetal, stillbirths, newborns, and infants up to approximately one year of age. Collection of 112 specimens was transferred to the Cleveland Museum of Natural History on a permanent loan in 1973.
|
|
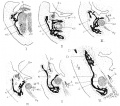
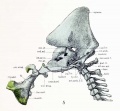
| 1921 43 mm Fetal Skull
|
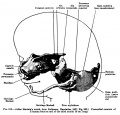
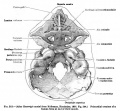
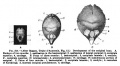
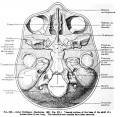
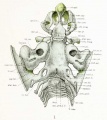
Fig. 1. Dorsal aspect of base of the cartilaginous skull with the basioccipital in the horizontal plane.
Fig. 2. Right half of dorsal aspect of the base of the cartilaginous skull.
Fig. 3. Dorsal aspect of cartilaginous and membranous skull.
Fig. 4. Dorsal aspect of base of the adult skull.
Fig. 5. Median sagittal aspect of the cartilaginous skull.
Fig. 6. Ventral aspect of base of the cartilaginous skull.
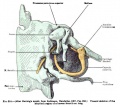
Fig. 7. Lateral aspect of cartilaginous skull and cervical vertebrae, with the brain and cervical cord and hypophysis in position.
Fig. 8. Lateral aspect of cartilaginous skull and cervical vertebra; with the brain, cervical cord, and nerves.
Fig. 9. Lateral view of cartilaginous skull and cervical vertebrae with the overlying membranous skull and the dorsal membrane.
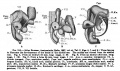
Fig. 10. Dorsal aspect of sphenoid cartilage, showing attachment of the orbital muscles to the basal part of the orbital wing.
Fig. 11. Dorsal aspect of sphenoid cartilage.
Fig. 12. Lateral view of the right otic region. Part of the malleus and incus cut away showing course of facial nerve and position of otic ganglion.
Fig. 13. Lateral view of right otic region showing relations of facial nerve.
Fig. 14. Lateral view of base of cartilaginous skull with deeper muscles of occipital region and of the mouth and pharynx.
Fig. 15. Lateral view of part of cartilaginous and membranous skull.
Fig. 16. Dorsal view of temporal and occipital cartilages, showing the relation of the inner ear to the otic capsule.
|
| 1918 Gray's Anatomy
|
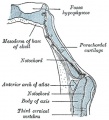
Sagittal section of cephalic end of notochord
Cartilaginous cranium (chondrocranium)
Human Embryo (CRL 8 cm) embryo model
Human Embryo (CRL 8 cm) embryo model from the left side
|
Terms
- anterior fontanel - developing skull region that closes by about 20 months postnatally.
- basion - anatomical region on the basiocciput located at the midpoint between the anterior margin and posterior margin (opisthion) of the foramen magnum.
- compound craniosynostosis premature suture fusion involving two or more sutures.
- craniosynostosis - (craniostenosis) the premature fusion of cranial sutures.
- dermatocranium - (membranous) skull calvarial vault develops from intramembranous ossification.
- harlequin eye - a term used to describe the prominent bilateral elliptical orbits of the skull seen in brachycephaly.
- endochondral ossification - bone formation from a pre-existing cartilage template, such as the chondrocranium.
- intramembranous ossification - bone formation from a membrane where no pre-existing cartilage is found, such as the calvarial vault component.
- neurocranium - the portion of the skull that surrounds the brain. Ossification of bones in cranial base (endochondral) and vault (intramembranous).
- opisthion - anatomical region located on the occipital bone, located at the midpoint of the posterior margin of the foramen magnum.
- posterior fontanel - developing skull region that closes by about 3 months postnatally.
- primary craniosynostosis - an intrinsic defect in a suture.
- secondary craniosynostosis - premature closure of normal sutures due to systemic and metabolic (hyperthyroidism, hypercalcemia, hypophosphatasia, vitamin D deficiency, renal osteodystrophy, Hurler's Syndrome, sickle cell disease and thalassemia) and those that can affect brain growth.
- simple craniosynostosis - premature fusion involving only one suture.
- synostosis - premature fusion.
- viscerocranium - facial skeleton and some anterior neck structures.
External Links
External Links Notice - The dynamic nature of the internet may mean that some of these listed links may no longer function. If the link no longer works search the web with the link text or name. Links to any external commercial sites are provided for information purposes only and should never be considered an endorsement. UNSW Embryology is provided as an educational resource with no clinical information or commercial affiliation.
- Johns Hopkins Fetal Skull Collection (1918–1951) - collection was begun by Adolph Hans Schultz (1891–1976) - fetal, stillbirths, newborns, and infants up to approximately one year of age. Collection of 112 specimens was transferred to the Cleveland Museum of Natural History on a permanent loan in 1973.
| Johns Hopkins Fetal Skull Collection (1918–1951)
|
| Johns Hopkins Fetal Skull Collection (1918–1951) - Simplified | Simplified Collapse | Full | Skull Development
|
| Specimen
|
Schultz Number
|
Schultz Number (Old)
|
Sex
|
Race
|
Ted Combs Age 1
|
Ted Combs Age 2
|
Ted Combs Notes
|
| JH 001
|
6
|
Blank
|
Male
|
B
|
5-6
|
IU
|
Left Occipital Condyle Missing 7/01 JR
|
| JH 002
|
15
|
253
|
Male
|
B
|
7
|
IU
|
|
| JH 003
|
18
|
Blank
|
Male
|
B
|
11
|
PN
|
LEFT GREATER WING MAY HAVE BEEN BROKEN
|
| JH 004
|
34
|
394
|
Male
|
B
|
12
|
PN
|
ENTIRE BASICRANIUM FUSED
|
| JH 005
|
35
|
361
|
Male
|
B
|
10
|
IU
|
|
| JH 006
|
36
|
258
|
Male
|
B
|
7
|
IU
|
ADOLF H SCHULTZ DRAWING INCLUDED
|
| JH 007
|
38
|
269
|
Male
|
B
|
10-11
|
IU
|
IMPROPER OSSIFICATION OF DORSUM STELLA
|
| JH 008
|
51
|
Blank
|
Male
|
B
|
5
|
IU
|
NOT ALL BONES BELONG HERE
|
| JH 009
|
56
|
271
|
Male
|
B
|
10
|
IU
|
|
| JH 010
|
58
|
340
|
Male
|
B
|
9-10
|
IU
|
|
| JH 011
|
62
|
Blank
|
Male
|
B
|
0
|
Newborn
|
|
| JH 012
|
67
|
322
|
Male
|
B
|
0
|
Newborn
|
MOLAR BUDS INCLUDED
|
| JH 013
|
69
|
299
|
Male?
|
B
|
9
|
IU
|
CHECK SEX
|
| JH 014
|
71
|
323
|
Male
|
B
|
0
|
Newborn
|
|
| JH 015
|
78
|
298
|
Male
|
B
|
8
|
IU
|
IMPROPER OSSIFICATION OF THE STELLA TURCICA
|
| JH 016
|
83
|
Blank
|
Male
|
B
|
7
|
IU
|
|
| JH 017
|
91
|
334
|
Male
|
B
|
10
|
IU
|
|
| JH 018
|
96
|
310
|
Male
|
B
|
10
|
IU
|
SQUAMOUS PORTION OF OCCIPITAL IN 2 PIECES
|
| JH 019
|
109
|
315
|
Male
|
B
|
10
|
IU
|
EXTRA BROKEN MALLEUS INCLUDED
|
| JH 020
|
110
|
257
|
Male
|
B
|
6
|
IU
|
TEMPORALS POORLY OSSIFIED
|
| JH 021
|
111
|
342
|
Male
|
B
|
3
|
PN
|
|
| JH 022
|
126
|
367
|
Male
|
B
|
10
|
IU
|
|
| JH 023
|
135
|
250
|
Male
|
B
|
8
|
IU
|
VERY YOUNG
|
| JH 024
|
137
|
285
|
Male
|
B
|
8
|
IU
|
|
| JH 025
|
139
|
400
|
Male
|
B
|
0
|
Newborn
|
|
| JH 026
|
144
|
Blank
|
Male
|
B
|
10
|
IU
|
"Two right lateral occipital bones and no left
JR 7/12/2001"
|
| JH 027
|
147
|
391
|
Male
|
B
|
2
|
PN
|
LEFT FRONTAL IS THE ONLY BONE PRESENT.
|
| JH 028
|
155
|
355
|
Male
|
B
|
0
|
Newborn
|
|
| JH 029
|
159
|
273
|
Male
|
B
|
9
|
IU
|
|
| JH 030
|
161
|
367
|
Male
|
B
|
0
|
Newborn
|
|
| JH 031
|
164
|
359
|
Male
|
B
|
2
|
PN
|
MANDIBLE ONCE FUSED, NOW BROKEN"
|
| JH 032
|
178
|
483
|
Male
|
B
|
15
|
PN
|
MaleOST OF BASICRANIUM FUSED
|
| JH 033
|
184
|
365
|
Male
|
B
|
2
|
PN
|
|
| JH 034
|
189
|
377
|
Male
|
B
|
3
|
PN
|
|
| JH 035
|
2
|
306
|
Female
|
B
|
0
|
Newborn
|
MANDIBLE WAS FUSED: NOW BROKEN
|
| JH 036
|
8
|
Blank
|
Female
|
B
|
9
|
IU
|
|
| JH 037
|
14
|
236
|
Female
|
B
|
5
|
IU
|
|
| JH 038
|
17
|
Blank
|
Female
|
B
|
14
|
PN
|
ADOLF H SCHULTZ DRAWING INCLUDED
|
| JH 039
|
44
|
298
|
Female
|
B
|
8
|
IU
|
EXTRA MALLEUS
|
| JH 040
|
45
|
Blank
|
Female
|
B
|
0
|
Newborn
|
POOR OSSIFICATION OF THE CALVARIA
|
| JH 041
|
53
|
440
|
Female
|
B
|
12
|
PN
|
WHOLE SKULL BADLY OSSIFIED
|
| JH 042
|
57
|
366
|
Female
|
B
|
2
|
PN
|
|
| JH 043
|
59
|
Blank
|
Female
|
B
|
8
|
IU
|
|
| JH 044
|
61
|
340
|
Female
|
B
|
9
|
IU
|
INCOMPLETE
|
| JH 045
|
63
|
340BUG!!!
|
Female
|
B
|
12
|
PN
|
TEETH BELONG TO JH 05. BAD BONE.
|
| JH 046
|
70
|
345
|
Female
|
B
|
3
|
PN
|
|
| JH 047
|
75
|
364
|
Female
|
B
|
0
|
Newborn
|
|
| JH 048
|
84
|
Blank
|
Female
|
B
|
8
|
IU
|
|
| JH 049
|
86
|
341
|
Female
|
B
|
2
|
PN
|
|
| JH 050
|
88
|
294
|
Female
|
B
|
8
|
IU
|
|
| JH 051
|
101
|
290
|
Female
|
B
|
8
|
IU
|
|
| JH 052
|
107
|
Blank
|
Female
|
B
|
8
|
IU
|
|
| JH 053
|
118
|
311
|
Female
|
B
|
9
|
IU
|
NASAL BONES FUSED
|
| JH 054
|
120
|
252
|
Female
|
B
|
8
|
IU
|
|
| JH 055
|
121
|
276
|
Female
|
B
|
6
|
IU
|
|
| JH 056
|
122
|
313
|
Female
|
B
|
?
|
?
|
TWO FRONTALS FROM TWO SPECIMENS (SIDES IN DISPUTE) EAR OSSICLES WITH SMALL....(?)
|
| JH 057
|
127
|
307
|
Female
|
B
|
10
|
IU
|
|
| JH 058
|
132
|
354
|
Female
|
B
|
4
|
PN
|
|
| JH 059
|
149
|
290
|
Female
|
B
|
8
|
IU
|
|
| JH 060
|
150
|
2825
|
Female
|
B
|
See Note
|
See Note
|
Age estimated as 8 months to Newborn
|
| JH 061
|
169
|
340
|
Female
|
B
|
0
|
Newborn
|
|
| JH 062
|
172
|
283
|
Female
|
B
|
7
|
IU
|
|
| JH 063
|
185
|
345
|
Female
|
B
|
10
|
IU
|
|
| JH 064
|
190
|
331
|
Female
|
B
|
2
|
PN
|
|
| JH 065
|
191
|
256
|
Female
|
B
|
5-6
|
IU
|
|
| JH 066
|
10
|
240
|
Male
|
W
|
5
|
IU
|
|
| JH 067
|
20
|
Blank
|
Male
|
W
|
0
|
Newborn
|
Reported missing by JR 7/001
|
| JH 068
|
40
|
Blank
|
Male
|
W
|
2
|
PN
|
|
| JH 069
|
48
|
340
|
Male
|
W
|
7
|
IU
|
|
| JH 070
|
49
|
274
|
Male
|
W
|
6-7
|
IU
|
|
| JH 071
|
74
|
332
|
Male
|
W
|
10
|
IU
|
|
| JH 072
|
77
|
336
|
Male
|
W
|
10
|
IU
|
|
| JH 073
|
89
|
344
|
Male
|
W
|
9
|
IU
|
|
| JH 074
|
92
|
279
|
Male
|
W
|
6
|
IU
|
|
| JH 075
|
105
|
Blank
|
Male
|
W
|
6
|
IU
|
|
| JH 076
|
108
|
280
|
Male
|
W
|
9
|
IU
|
|
| JH 077
|
129
|
340
|
Male
|
W
|
1
|
PN
|
|
| JH 078
|
131
|
364
|
Male
|
W
|
9
|
IU
|
|
| JH 079
|
136
|
363
|
Male
|
W
|
9
|
IU
|
|
| JH 080
|
138
|
355
|
Male
|
W
|
3
|
PN
|
KERKRING'S CENTER OBSERVED
|
| JH 081
|
141
|
347
|
Male
|
W
|
2
|
PN
|
MANDIBLE ONCE FUSED NOW BROKEN
|
| JH 082
|
143
|
326
|
Male
|
W
|
0
|
Newborn
|
EXTRA MALLEUS INCLUDED
|
| JH 083
|
146
|
320
|
Male
|
W
|
9
|
IU
|
THREE PARIETAL FRAGMENTS
|
| JH 084
|
151
|
353
|
Male
|
W
|
3
|
PN
|
|
| JH 085
|
156
|
364
|
Male
|
W
|
2
|
PN
|
|
| JH 086
|
157
|
288
|
Male
|
W
|
8
|
IU
|
|
| JH 087
|
162
|
374
|
Male
|
W
|
9
|
IU
|
|
| JH 088
|
166
|
382
|
Male
|
W
|
4
|
PN
|
MANY TOOTH FRAGMENTS
|
| JH 089
|
171
|
380
|
Male
|
W
|
10
|
IU
|
NASAL BONES FUSED
|
| JH 090
|
179
|
Blank
|
Male
|
W
|
3
|
PN
|
|
| JH 091
|
186
|
373
|
Male
|
W
|
9
|
IU
|
|
| JH 092
|
188
|
Blank
|
Male
|
W
|
8
|
IU
|
|
| JH 093
|
192
|
328
|
Male
|
W
|
7
|
IU
|
KERKRING'S CENTER OBSERVED
|
| JH 094
|
13
|
Blank
|
Female
|
W
|
0
|
Newborn
|
TEETH FRAGMENTS
|
| JH 095
|
23
|
352
|
Female
|
W
|
4
|
PN
|
TYMPANIC MEMBRANE INTACT
|
| JH 096
|
43
|
268
|
Female
|
W
|
5
|
IU
|
ADOLF H SCHULTZ DRAWING INCLUDED
|
| JH 097
|
47
|
313
|
Female
|
W
|
8
|
IU
|
ONE BONE FRAGMENT - SQUAMOUS TYPE
|
| JH 098
|
64
|
364
|
Female
|
W
|
3
|
PN
|
|
| JH 099
|
95
|
350
|
Female
|
W
|
4
|
PN
|
HYDROCEPHALIC
|
| JH 100
|
100
|
365
|
Female
|
W
|
0
|
Newborn
|
|
| JH 101
|
114
|
396
|
Female
|
W
|
5
|
PN
|
MANDIBLE ONCE FUSED NOW BROKEN
|
| JH 102
|
116
|
400
|
Female
|
W
|
2
|
PN
|
TEETH NOT COUNTED
|
| JH 103
|
117
|
290
|
Female
|
W
|
7
|
IU
|
TWO TOOTH BUDS
|
| JH 104
|
128
|
368
|
Female
|
W
|
5
|
PN
|
TOOTH FRAGMENTS
|
| JH 105
|
134
|
Blank
|
Female
|
W
|
9
|
IU
|
EAR OSSICLES PRESENT - NO COUNT
|
| JH 106
|
148
|
290
|
Female
|
W
|
8
|
IU
|
EAR OSSICLES PRESENT - NO COUNT
|
| JH 107
|
160
|
60
|
Female
|
W
|
2
|
PN
|
EAR OSSICLES PRESENT - NO COUNT
|
| JH 108
|
167
|
372
|
Female
|
W
|
1
|
PN
|
EAR OSSICLES PRESENT - NO COUNT
|
| JH 109
|
168
|
316
|
Female
|
W
|
8
|
IU
|
EAR OSSICLES PRESENT - NO COUNT
|
| JH 110
|
170
|
331
|
Female
|
W
|
0
|
Newborn
|
EAR OSSICLES PRESENT - NO COUNT
|
| JH 111
|
175
|
342
|
Female
|
W
|
10
|
IU
|
EAR OSSICLES PRESENT - NO COUNT
|
| JH 112
|
194
|
317
|
Female
|
W
|
8
|
IU
|
|
| Johns Hopkins Fetal Skull Collection (1918–1951) - The collection was begun by Adolph Hans Schultz (1891–1976) - fetal, stillbirths, newborns, and infants up to approximately one year of age. Collection of 112 specimens was transferred to the Cleveland Museum of Natural History on a permanent loan in 1973.
|
|
Glossary Links
- Glossary: A | B | C | D | E | F | G | H | I | J | K | L | M | N | O | P | Q | R | S | T | U | V | W | X | Y | Z | Numbers | Symbols | Term Link
Cite this page: Hill, M.A. (2024, April 20) Embryology Musculoskeletal System - Skull Development. Retrieved from https://embryology.med.unsw.edu.au/embryology/index.php/Musculoskeletal_System_-_Skull_Development
- What Links Here?
- © Dr Mark Hill 2024, UNSW Embryology ISBN: 978 0 7334 2609 4 - UNSW CRICOS Provider Code No. 00098G