ANAT2341 Lab 1 - Spermatogenesis
From Embryology
| ANAT2341 Lab 1: Introduction | Gametogenesis | Oogenesis | Spermatogenesis | Fertilization | Sex Determination | Online Assessment | ANAT2341 Lab 1 - Quiz |
Human Spermatozoa Development
- Spermatogenesis is the process of spermatagonia (diploid) mature into spermatozoa (haploid).
- Spermioogenesis is a part of spermatogenesis where round spermatids mature into the mature spermatozoa form.
- Continuously throughout life occurs in the seminiferous tubules in the male gonad- testis (plural testes).
- At puberty spermatagonia activate and proliferate (mitosis).
- about 48 days from entering meiosis until morphologically mature spermatozoa
- about 64 days to complete spermatogenesis, depending reproduction time of spermatogonia
- Follicle stimulating hormone (FSH) - stimulates the spermatogenic epithelium
- Luteinizing-hormone (LH) - stimulates testosterone production by Leydig cells
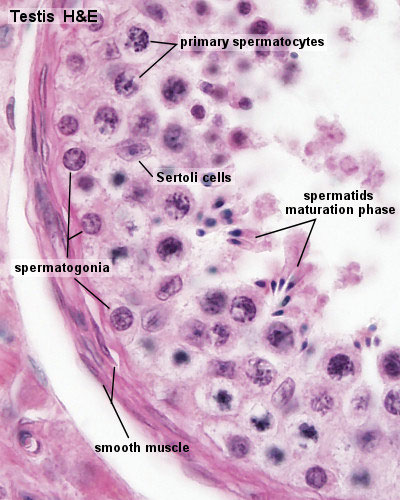
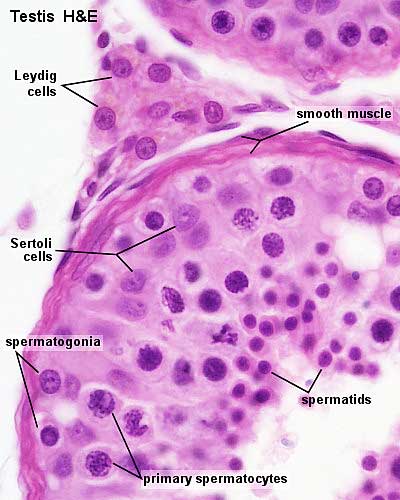
Seminiferous Tubule
- Spermatogonia - are the first cells of spermatogenesis
- Primary spermatocytes - large, enter the prophase of the first meiotic division
- Secondary spermatocytes - small, complete the second meiotic division
- Spermatid - immature spermatozoa
- Spermatozoa - differentiated gamete
- Spermatozoa development: primordial germ cell - spermatogonia - primary spermatocyte - secondary spermatocytes - spermatid - spermatozoa
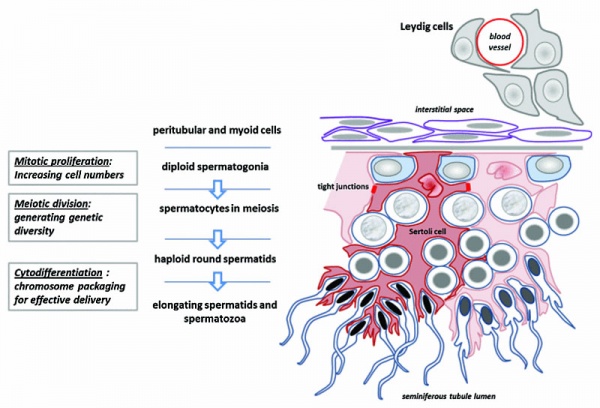
Seminiferous tubule cartoon[1]
Spermatozoa
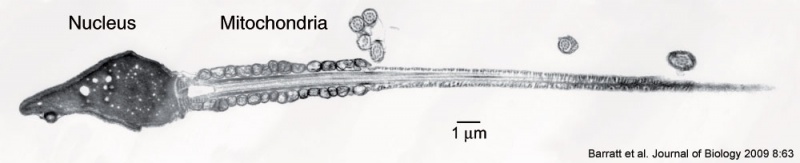
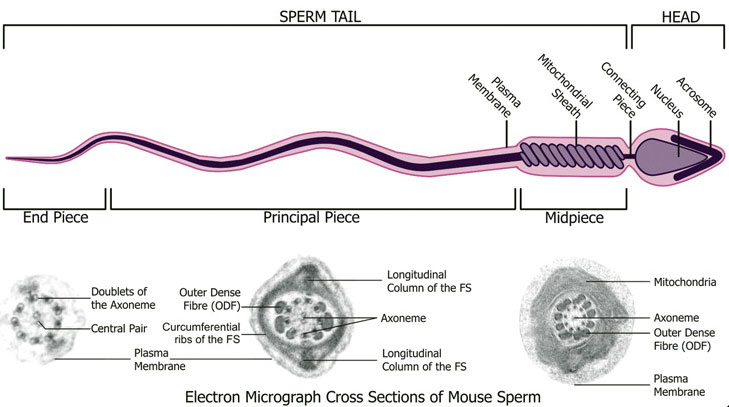
Spermatozoa Structure
Spermatozoa (mouse) cross-sections of tail (EM) and diagram[2]
Puberty
- In humans at puberty, hormonal and morphological changes occur within the gonad and other systems (secondary sex characteristics).
- Within the testis the immature Sertoli cells cease to proliferate and differentiate.
- Spermatogonium proliferate and spermatogenesis begins.
- It takes about 70 days for cells to mature from the diploid spermatogonium to a primary spermatocyte.
- This maturation occurs in waves along the seminiferous tubules.
- Links: Puberty
Ejeculate
- release of spermatozoa and accessory gland secretions from the male genital tract (3.5 ml)
- 200-600 million sperm, by volume less than 10 % spermatozoa
- Accessory Gland secretions - 60 % seminal vesicle, 30 % prostate and 10 % bulbourethral
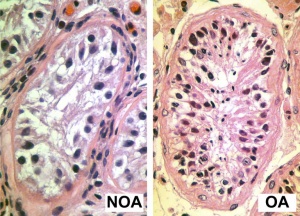
Male Abnormalities
- Oligospermia - (Low Sperm Count) less than 20 million sperm after 72 hour abstinence from sex
- Azoospermia - (Absent Sperm) blockage of duct network
- Immotile Cilia Syndrome - lack of sperm motility
- Links: Spermatozoa Development | MBoC - Sperm | MBoC - Highly simplified drawing of a cross-section of a seminiferous tubule in a mammalian testis | MBoC - Cytoplasmic bridges in developing sperm cells and their precursors
| 2011 Lab 1: Introduction | Gametogenesis | Oogenesis | Spermatogenesis | Fertilization | Online Assessment |
Terms
- sperm - See spermatozoa. The male haploid reproductive cell, often used generically (and incorrectly) to describe these cells and the fluid of the ejaculate. Term is a shortened form of scientifically correct term spermatazoa.
- sperm annulus - (Jensen's ring; Latin, annulus = ring) A region of the mammalian sperm flagellum connecting the midpiece and the principal piece. The annulus is a septin-based structure formed from SEPT1, 4, 6, 7 and 12. Septins are polymerizing GTPases that can act as a scaffold forming hetero-oligomeric filaments required for cytokinesis and other cell cycle roles.
- spermatid - Intermediate cell in spermatozoa development, within the testis seminiferous tubule they lie in the luminal cell layer to the secondary spermatocyte. These small cells are haploid and in spermiogenesis change their cellular structure and shape to form spermatozoa.
- (More? Spermatozoa Development | Testis Development | Fertilization | Lecture - Cell Division/Fertilization)
- spermatogenesis - (Greek, genesis = origin, creation, generation) The term used to describe the process of diploid spermatagonia division and differentiation to form haploid spermatazoa within the testis (male gonad). The process includes the following cellular changes: meiosis, reoorganization of DNA, reduction in DNA content, reorganization of cellular organelles, morphological changes (cell shape). The final process of change in cell shape is also called spermiogenesis.
- spermiogenesis - (Greek, genesis = origin, creation, generation) The maturation process of the already haploid spermatids into the mature spermatozoa shape and organization. This process involves reorganization of cellular organelles (endoplasmic reticulum, Golgi apparatus, mitochondria), cytoskeletal changes (microtubule organization) and morphological changes (cell shape, acrosome and tail formation). The process of maturation of the spermatids into spermatozoa: chromatin condenses, nucleus becomes smaller, the Golgi apparatus is modified to form the acrosome, microtubules are reorganised to form the tail, mitochondria are relocated to the initial segment of the tail and the majority of cell cytoplasm is discarded.
- spermatogonia - These cells form in the embryo from the primordial germ cell and are located in the seminiferous tubule adjacent to the basal membrane. The cells can either divide and separate to renew the stem cell population, or they divide and stay together as a pair (Apr spermatogonia) connected by an intercellular cytoplasmic bridge to begin to differentiate and eventually form spermatazoa.
- spermatozoa - (spermatozoon, singular term) The male haploid gamete cell produced by meiosis in the testis (male gonad) seminiferous tubule. In humans, produced from puberty onwards and develop from the diploid stem cell the spermatogonia. The developmental meiosis is called spermatogenesis and the final morphologiccal (shape) change is called spermeiogenesis. The mature human spermatozoon formed from the spermatid has a head, neck and tail and is about 60 µm long. At ejaculation these cells undergo capacitation are activated and become motile.
- spermatozoa head - Following spermiogenesis, the first region of the spermatozoa containing the haploid nucleus and acrosome. In humans, it is a flattened structure (5 µm long by 3 µm wide) with the posterior part of nuclear membrane forming the basal plate region. The human spermatozoa is about 60 µm long, actively motile and divided into 3 main regions (head, neck and tail).
- spermatozoa neck - Following spermiogenesis, the second region of the spermatozoa attached to basal plate, transverse oriented centriole, contains nine segmented columns of fibrous material, continue as outer dense fibres in tail. In humans, it forms a short structure (1 µm). The human spermatozoa is about 60 µm long, actively motile and divided into 3 main regions (head, neck and tail).
- spermatozoa tail - Following spermiogenesis, the third region of the spermatozoa that has a (head, neck and tail). The tail is also divided into 3 structural regions a middle piece, a principal piece and an end piece. In humans: the middle piece (5 µm long) is formed by axonema and dense fibres surrounded by mitochondria; the principal piece (45 µm long) fibrous sheath interconnected by regularly spaced circumferential hoops; the final end piece (5 µm long) has an axonema surrounded by small amount of cytoplasm and plasma membrane.
- spermatogonial stem cells - (SSCs) The spermatagonia cells located beside the seminiferous tubule basal membrane that either divide and separate to renew the stem cell population, or they divide and stay together as a pair (Apr spermatogonia) connected by an intercellular cytoplasmic bridge to differentiate and eventually form spermatazoa.
- sperm protein 56 - A component of the spermatozoa acrosomal matrix released to the sperm surface during capacitation.
References
- ↑ <pubmed>22553488</pubmed>| PMC3341244 | Spermatogenesis
- ↑ <pubmed>19758979</pubmed>| PMC2816191 | Hum Reprod Update.
| ANAT2341 Lab 1: Introduction | Gametogenesis | Oogenesis | Spermatogenesis | Fertilization | Sex Determination | Online Assessment | ANAT2341 Lab 1 - Quiz |
Glossary Links
- Glossary: A | B | C | D | E | F | G | H | I | J | K | L | M | N | O | P | Q | R | S | T | U | V | W | X | Y | Z | Numbers | Symbols | Term Link
Cite this page: Hill, M.A. (2024, April 23) Embryology ANAT2341 Lab 1 - Spermatogenesis. Retrieved from https://embryology.med.unsw.edu.au/embryology/index.php/ANAT2341_Lab_1_-_Spermatogenesis
- © Dr Mark Hill 2024, UNSW Embryology ISBN: 978 0 7334 2609 4 - UNSW CRICOS Provider Code No. 00098G